 
The Health Connector is also planning to bolster its staff for the coming wave of new members. 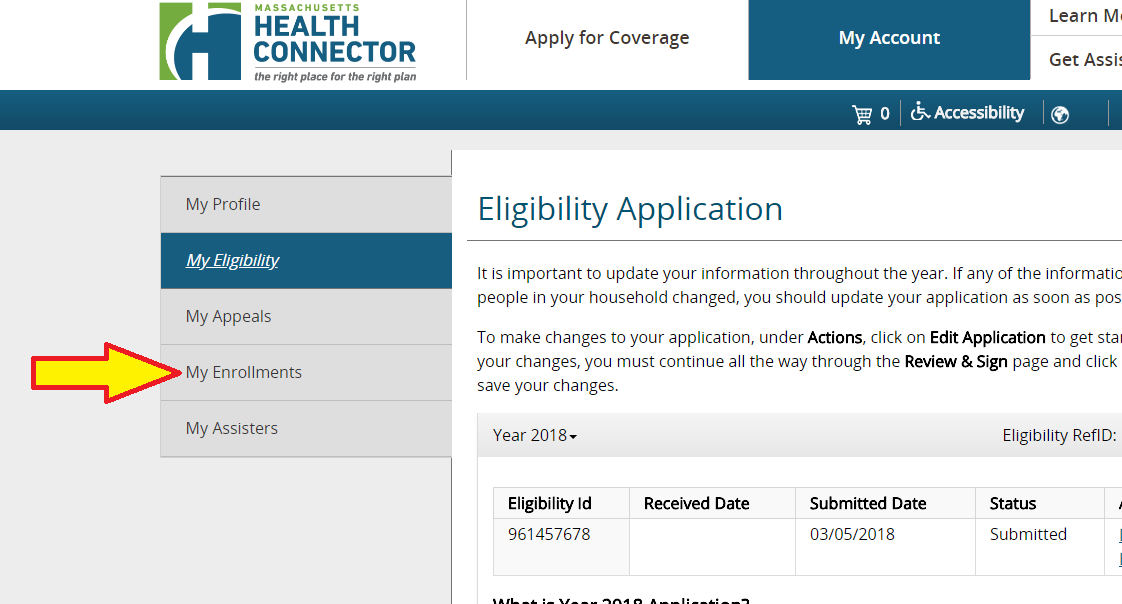
The authority is working with MassHealth to create an “integrated eligibility system,” so someone who is notified of a MassHealth termination online can immediately begin the process of using the Health Connector to find a new plan, Lefferts said.Īfter notice of termination, individuals will have until the end of the following month on MassHealth, meaning, if someone were alerted in February that they would lose their insurance, they would need to find a new plan by March 31 for uninterrupted coverage. People cut off from MassHealth will be messaged once a week for two months, and then three times a month after that, communications director Jason Lefferts said at the board meeting. The Health Connector is opening a special enrollment period from April through November for those who lost MassHealth coverage to make the transition “as smooth as possible,” Director of Policy and Applied Research Marissa Woltmann said at a Health Connector board meeting Thursday morning. Starting with 294,584 members in January 2020, the Health Connector was down to 214,102 members as of January 2023. Meanwhile, the number of Bay Staters using the Connector has declined as more people have qualified for government-funded plans. The program is the largest in state government and is jointly funded by the state and the feds. Since the start of the pandemic, MassHealth enrollment has increased by a third, up from 1,750,966 in December 2019 to 2,337,799 members in December 2022. As Bay Staters who qualified under COVID-19 provisions lose their MassHealth coverage, the Health Connector Authority, which aims to connect people in need with affordable health plans, is preparing for up to 200,000 new members. The federal emergency is due to come to a close this spring.Ĭontinuous Medicaid enrollment ends on March 31, and the federal government is phasing out pandemic-era enhanced funds this year. You will now be on the Eligibility Application screen where you can view your current application details, report changes to your current application, and submit any requested information.The state program that helps people acquire required health insurance policies is preparing for an influx of new enrollees as enhanced federal funds for Medicaid are scheduled to be cut off in March.Īt the start of the pandemic, Congress required that state Medicaid programs keep people continuously enrolled through the end of the month in which the COVID-19 public health emergency ended. View application details, report changes, and submit information On the Validate Invitation Code screen you need to enter your invitation code (if it isn’t already filled in) and your date of birth, then click Next.Ĩ. Verify your email and enter your invitation code Enter your confirmation code and click Nextħ. Check your spam or junk email folder if you do not see the email from MA Login.Ħ.  
You will need to confirm your email address before you can use your MA Login account. Once you click the Continue button, check your email. Make sure to write down your username, password, and security question answers. You will be redirected to the MA HIX webpage to create your account when you validate your invitation code.īefore you hit Continue, don’t forget to make sure that all of your information is correct. The email will also include a link to validate your code on the account sign in page labeled My Account. We will confirm your email address and send your invitation code via email with the subject line “ Take Action: Enter your Health Connector account invitation code.” Check your spam or junk email folder if you do not see the email. If you don’t have a recent notice, you can get help with MA Login by calling (844) 365-1841 or TDD/TTY 711. You can find your invitation code on your most recent MassHealth notice. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
